This is one in a series of articles that provide detailed and updated information about Dentin.
In this specific article, which focuses on Dentin – Exposure and Tooth Wear, you can read about:
- Dentin Exposure and Tooth Wear
- How Does Dentin Get Exposed?
- Dentin Exposure Symptoms: What Happens if Dentin is Exposed?
- Dentin Exposure Treatment: How So You Fix Exposed Dentin?
- Dentin Loss
- What Causes Dentin Loss?
- Tooth Fillings
- Dentin Grinder
- Dentin Graft
- What is a Dentin Pin?
- Direct and Indirect Pulp Capping
- Dentin Biomimetics and Tissue Engineering
- Dentin Regeneration and Growth Factors
- Dentin and Nutritional Factors
For additional articles about Dentin, see the Topic Menu.
Dentin Exposure and Tooth Wear
Dentin exposure and tooth wear are closely related dental issues that can affect an individual’s oral health and overall well-being. Tooth wear can affect both the enamel and dentin layers, but dentin is more susceptible to wear due to its lower mineral content and increased porosity compared to enamel. Dentin is a layer of the tooth found beneath the enamel and contains tiny tubules that lead to the nerves of the tooth. When dentin becomes exposed, it can lead to increased sensitivity, pain, and a higher risk of tooth decay.
Tooth wear refers to the loss of dental hard tissue due to chemical and physical factors, rather than bacterial factors. Tooth wear can affect both the enamel and dentin layers, but dentin is more susceptible to wear due to its lower mineral content and increased porosity compared to enamel.
Tooth wear can be caused by a variety of factors, including:
- Abrasion – such as from toothbrushing
- Erosion – from acidic foods and beverages
- Attrition – from tooth-to-tooth contact, such as grinding or clenching
- Abfraction – from stress on the tooth structure
In most cases, tooth wear is multifactorial, involving a combination of various causes. For example, abrasion from toothbrushing rarely causes tooth wear, but it becomes more susceptible after an acid challenge. Following tooth wear – natural repair processes take place. However, when tooth wear progresses faster than normal for a particular age due to excessive stimulation, it is considered pathological tooth wear.
When tooth wear becomes more severe, it can lead to dentin exposure. The protective enamel layer, which is harder and more mineralized, is lost or damaged, leaving the underlying dentin exposed. This exposure can result in increased sensitivity to temperature, pressure, and sweet or acidic substances, as the tubules in the dentin are more directly connected to the tooth’s nerves. Dentin exposure is an important turning point in the process of dental tissue loss.
Preventing dentin exposure and tooth wear involves maintaining good oral hygiene practices, such as brushing with a soft-bristled toothbrush, using a toothpaste containing fluoride, and flossing regularly. Additionally, limiting the consumption of acidic and sugary foods and beverages, avoiding tooth grinding or clenching, and seeking treatment for conditions like acid reflux can help prevent excessive tooth wear.
Regular dental check-ups are crucial for early detection and management of tooth wear and dentin exposure. Dentists can monitor the progression of wear, provide preventive measures, and recommend appropriate treatments, such as dental bonding, restorations, or the use of desensitizing toothpaste, to help preserve the tooth structure and alleviate any discomfort. Early diagnosis and continuous monitoring of tooth wear progression are valuable for delaying or inhibiting the initiation of restorative treatment.
How Does Dentin Get Exposed?
Dentin is protected by a layer of hard, mineralized enamel. When the enamel layer is damaged or lost, dentin, which is not as hard as enamel and contains nerve endings connected to the pulp, becomes exposed. Dentin exposure leads to symptoms like sensitivity when consuming hot or cold foods.
Some common causes of enamel damage and dentin exposure include:
- Overzealous Brushing: Dentists recommend using a soft-bristled brush and brushing gently in a circular motion. Forceful brushing or using a hard-bristled toothbrush can wear down the enamel, exposing the underlying dentin. Repeated scrubbing with a hard toothbrush can also thin the enamel along the gum line, making it more susceptible to damage.
- Teeth Grinding (bruxism): This condition, often caused by stress or malocclusion, occurs when the upper and lower teeth clench and grind together, resulting in wear and tear, chips, and cracks. Over time, the protective enamel layer thins, and the dentin becomes exposed.
- Acidic Foods: The acidic content of citrus fruits can demineralize enamel, leading to dentin exposure.
- Gum Recession: Improper oral hygiene habits can cause food debris to remain stuck between teeth, leading to plaque buildup. This accumulation of bacteria-filled plaque results in gingivitis, a gum infection that can progress, cause gum recession, and expose dentin.
- Tooth Decay: Bacteria create cavities by secreting acid onto the tooth, which erodes the enamel layer. Once the enamel is gone, the dentin becomes exposed.
- GERD (Gastroesophageal Reflux Disease): Individuals with GERD are at risk for dentin exposure, as the acids that come back up their throat interact with enamel and cause demineralization. Constant exposure to acid can wear through the enamel, revealing the layer beneath it.
Addressing the factors that contribute to enamel damage and dentin exposure can help prevent tooth sensitivity and protect overall oral health.
Dentin Exposure Symptoms: What Happens if Dentin is Exposed?
When the protective enamel layer wears away or becomes damaged, the underlying dentin becomes exposed, leading to the following symptoms:
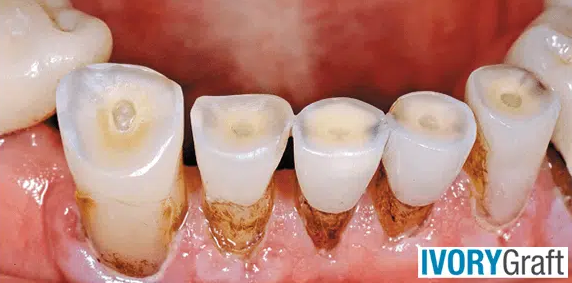
- Discoloration: Exposed dentin can cause brown, black, or white staining on the tooth surfaces. This discoloration may be more noticeable on the chewing surfaces or along the gumline.
- Tooth sensitivity: One of the most common symptoms of dentin exposure is tooth sensitivity, which can manifest as mild to sharp pain when consuming hot, cold, sweet, or acidic foods and beverages. This sensitivity occurs because the exposed dentinal tubules transmit external stimuli directly to the nerves in the pulp.
- Visible holes or pits: Exposed dentin may be accompanied by visible holes or pits in the teeth, indicating enamel erosion or cavities.
- Pain when biting down: Dentin exposure can cause discomfort or pain when biting down or applying pressure on the affected tooth. This pain may be intermittent or persistent, depending on the extent of the exposure.
- Toothache or spontaneous pain: In some cases, exposed dentin can lead to toothaches or spontaneous pain that occurs without any apparent cause. This pain might be dull, throbbing, or sharp, and it may be exacerbated by external stimuli or changes in temperature.
- Increased plaque and tartar buildup: Exposed dentin is more porous than enamel and can be more susceptible to plaque and tartar buildup. This can further increase the risk of tooth decay, gum disease, and other oral health problems.
Dentin exposure symptoms can vary depending on the severity and extent of the exposed dentin. If you experience any of these symptoms, it is crucial to consult a dentist to determine the cause of the dentin exposure and receive appropriate treatment to prevent further damage and alleviate discomfort.
Dentin Exposure Treatment: How So You Fix Exposed Dentin?
The primary goal of treating exposed dentin is to block the transmission of pain stimuli to the pulp. All available treatments aim to achieve this by either covering the exposed dentin and blocking the dentinal tubules or by desensitizing the nerves in the dental pulp to reduce pain signal transmission to the brain.
Various treatment options include:
- Painkillers: These medications can offer temporary relief by blocking nerve signaling, but a visit to the dentist for proper treatment of the dentin exposure is necessary for long-term resolution.
- Desensitizing Toothpaste: Desensitizing toothpaste contains anti-sensitivity ingredients, such as potassium nitrate, which work by sealing off the tubules. This prevents external stimuli like cold, hot, sweet, and acidic substances from reaching the nerves. However, the anti-sensitivity effects only last while the toothpaste is being used and will subside once discontinued.
- Professional Desensitizers: In-office desensitizers, such as KoR desensitizer and Gluma, seal off exposed dentin. These products offer longer-lasting effects compared to desensitizing toothpaste but may still wear off after a few months.
- Bonding Agent: Applying a bonding agent to the exposed dentin area can help reduce sensitivity. However, the effects may be temporary, as the bonding agent can wear away over time due to tooth brushing.
- Tooth Filling: Restoring the tooth with dental restorative material can cover up exposed dentin by adding an additional protective layer.
- Dental Crown: This option is less conservative than a tooth filling, as it involves drilling and preparing the entire tooth. The dental crown covers the whole tooth, ensuring that no dentin remains exposed.
- Dental Veneer: A more conservative and less invasive option compared to a dental crown, veneers are thin shells made of porcelain or composite resin material that are bonded to the front surface of the tooth. This treatment requires removing only the front part of the tooth before covering the exposed dentin, thus improving both the appearance and sensitivity of the affected tooth while leaving the other facets of the tooth untouched.
In all cases, it is essential to consult a dental professional to determine the most appropriate treatment option for addressing exposed dentin. A combination of treatments may be required to achieve the best results and prevent further dental complications.
Dentin Loss
Dentin loss refers to the erosion or damage of the dentin layer, which is a hard dental tissue located above the pulp of a tooth. Dentin contains many tiny tubules called dental tubules, which, when exposed or damaged, compromise the protective covering above the pulp. As a result, any stimuli, such as cold or hot temperatures, are perceived by the pulp as pain, causing discomfort to the patient.
In addition to sensitivity, dentin loss can also make teeth appear darker or discolored, as the thinning or absence of enamel exposes the darker dentin layer underneath. This can occur due to various factors, such as tooth decay, tooth abrasion, tooth erosion, gum recession, aging, and trauma.
Maintaining good oral hygiene habits, like brushing twice a day, flossing daily, and using fluoride toothpaste, can help prevent tooth decay, a common cause of dentin loss. Avoiding acidic foods and drinks, using a soft-bristled toothbrush, and wearing a mouthguard during physical activities can also help protect teeth from damage and wear.
Once dentin loss has occurred, the following treatment options can be considered, depending on the underlying cause and extent of the damage. If the dentin loss is minor, the dentist may recommend desensitizing toothpaste or fluoride treatments to help protect the exposed dentin and reduce sensitivity. In more extensive cases, the dentist may recommend placing a dental filling or crown to restore the lost tooth structure and protect the underlying dentin.
What Causes Dentin Loss?
Dentin loss, which refers to the erosion or damage of the dentin layer, can occur due to a variety of factors. Some common causes of dentin loss include:
- Tooth Decay: When bacteria in the mouth produce acids that erode the enamel, they can eventually reach the underlying dentin, causing it to wear away.
- Overzealous Brushing: Dentists recommend using a soft-bristle brush and brushing gently in a circular motion. Brushing your teeth with too much force and using a hard-bristle toothbrush can abrade the enamel and expose the underlying dentin. Repeated scrubbing with a hard toothbrush can thin the enamel along the gum line, making it easily damaged.
- Teeth Grinding (Bruxism): This condition, commonly caused by stress and malocclusion, also occurs during sleep. Teeth grinding involves the upper and lower teeth clenching and grinding together, causing wear and tear, chips, and cracks. Over time, the protective enamel layer becomes thinner, and the dentin becomes exposed.
- Citrus Fruits: The acidic content of citrus fruits can cause the demineralization of enamel, thus exposing dentin.
- Gum Recession: Due to improper oral hygiene habits, food debris may remain stuck between teeth, accumulating dental plaque that coats the teeth. This substance is filled with bacteria, leading to gingivitis, a gum infection that, if left untreated, progresses and results in gum recession and dentin exposure.
- Aging: Over time, teeth naturally become more brittle and susceptible to wear and tear, which can lead to dentin loss.
- Trauma: Physical injury or trauma to the teeth can also cause dentin loss.
To minimize the risk of dentin loss, it’s essential to maintain good oral hygiene practices, use a soft-bristle toothbrush, avoid acidic foods and drinks, and visit your dentist regularly for check-ups and cleanings. If you experience any symptoms of dentin loss, such as sensitivity or pain, it’s essential to see your dentist for an evaluation and appropriate treatment.
Tooth Fillings
Tooth fillings are a common dental procedure used to restore teeth that have been damaged by decay, fractures, or wear. They help to maintain the tooth’s structural integrity, prevent further damage, and restore the tooth’s function and appearance.
The steps involved in filling a tooth include:
- Anesthesia (Optional): Depending on the case, the dentist may inject a local anesthetic into your gum to numb the area around your tooth, making it insensitive to pain as the affected tooth is filled.
- Drilling: This crucial step involves removing the decayed or defective part of the tooth and preparing it to receive the filling. A dentist may use a traditional drill, laser, or abrasion instrument for this step.
- Cleanup: The area is cleaned to create space for the filling.
- Liner Placement: If the tooth decay is deep, a protective liner made of composite resin or glass ionomer may be placed to safeguard the nerve and prevent inflammation.
- Filling Application: After applying the liner and cleaning the cavity, the restoration or filling is placed.
- Multilayered Filling Application: Tooth-colored material is applied in layers after removing the decayed parts.
- Light Curing: In the case of composite resin fillings, a light source is used to harden or cure the filling after each layer is applied.
- Shaping the Composite Resin Filling: Once the multilayered resin application is complete, the composite is manipulated to achieve the desired shape.
- Trimming Excess Material: A drill or sandpaper may be used to trim off any excess material.
- Polishing and Finishing: The final restoration process involves polishing the tooth-colored filling until it seamlessly matches the surrounding tooth structure.
There are several types of filling materials available, each with its own advantages and disadvantages.
- Amalgam fillings: Amalgam is a mixture of metals, including mercury, silver, tin, and copper. These fillings have been used for over a century and are known for their durability and affordability. However, they are not aesthetically pleasing due to their silver color and may raise concerns about mercury exposure, although the risk is considered minimal.
- Composite resin fillings: Composite resin fillings are made of a mixture of plastic and fine glass particles. They can be matched to the color of your natural teeth, making them an aesthetically pleasing option. These fillings bond directly to the tooth structure, providing additional support. However, composite resin fillings may not be as durable as amalgam fillings, especially in larger cavities.
- Glass ionomer fillings: Glass ionomer fillings are made from a combination of acrylic and glass materials. They release fluoride, which can help prevent further tooth decay. Glass ionomer fillings are often used for small cavities, especially in children or in areas that are not subject to heavy chewing pressure. They are not as durable as amalgam or composite resin fillings and may not be suitable for larger cavities.
- Ceramic fillings: Ceramic fillings, often made from porcelain, are both durable and aesthetically pleasing. They are resistant to staining and abrasion and can be color-matched to your natural teeth. However, they are more expensive than other filling options and may require more extensive tooth preparation.
- Gold fillings: Gold fillings are highly durable and well-tolerated by the gums. They can last for many years, but they are also the most expensive filling option and require multiple visits to complete the procedure.
The choice of filling material depends on factors such as the location and size of the cavity, the patient’s dental history, aesthetic preferences, and budget. Your dentist will recommend the most suitable filling material based on your individual needs and the specific requirements of your tooth restoration.
Dentin Grinder
Autogenous grafts are considered the “gold standard” of grafting material since they are derived from the patient’s own body. However, the need for a second surgical site (for example to harvest an autologous bone graft from the patient’s bone), often led to the selection of alternative grafts to avoid additional incisions and the increased risk of infection.
A dentin grinder is a specialized tool designed to grind extracted teeth into usable dentin for autogenous grafts. With a dentin grinder, dentists or periodontists can create autogenous grafting material from the patient’s own extracted teeth, which offers several advantages in terms of biocompatibility, healing, and a reduced risk of infection.
The extracted tooth is inserted into the grinder, which typically produces particulate dentin about three times the volume of the original tooth. Most dentin grinders come with a sterilization kit, allowing dental professionals to cleanse and sterilize the ground dentin before using it in a grafting procedure. Autogenous grafts pose a lower risk of infection, leading to improved patient outcomes and overall satisfaction after the procedure is completed.
Dentin Graft
A dentin graft is a type of bone grafting procedure that utilizes dentin, the major component of human teeth, as the grafting material. The human tooth is composed of 80% dentin, 15% enamel, and 5% cement and pulp. Dentin, which is the major component, has a composition very similar to bone, with the same high mineral content and tubular architecture. The morphogenetic protein of dentin can induce new bone formation and replace new bone without causing an inflammatory reaction.
Many biomaterials and synthetic materials used to repair hard and soft tissue defects are inexpensive and do not involve a biological risk. However, they lack the capacity for osteoconduction (providing a suitable environment that allows bone-forming cells, osteoblasts, to attach and proliferate) and osteoinduction (stimulating the differentiation of cells into osteoblasts), limiting their use in forming useful bone (osteoinduction).
In contrast, Dentin grafts, regarded as the new gold standard for dental bone grafting, support both osteoconduction and osteoinduction and therefore lead to more osteogenesis (bone creation). Dentin’s osteoinductive properties are partly attributed to the presence of bone morphogenic proteins (BMPs) in dentin. Dentin’s osteoconductive properties are attributed to its similarity in composition to bone (including calcium ions and organized phosphorus, such as hydroxyapatite and TCP) and to its micro-pores that are ideal for hosting osteoblasts.
Dentin also includes type I collagen and growth factors, which are essential for bone healing and regeneration. In addition, Dentin is known to directly undergo ankylosis, fusion to the surrounding bone, thus it excels for example in Periodontic treatment. Several studies conducted in the past have demonstrated that dentin can successfully enhance the process of bone formation.
Dentin graft can originate from grinded and cleansed teeth extracted from the patient (Autograft) or from animal (Xenograft). Ivory Graft is the first ever commercial and CE approved dentin xenograft, using porcine teeth as a source, and making the dentin advantages available to all dentists, even when no dentin autograft from patients’ extracted teeth is available.
What is a Dentin Pin?
A dentin pin, also known as a dental pin, is a small metal or plastic post used to anchor a dental restoration, such as a filling or crown, to the underlying dentin of a tooth. Dentin pins are typically employed when there is insufficient natural tooth structure remaining to support the restoration.
The process of placing a dentin pin involves drilling a small hole into the tooth’s dentin and inserting the pin into the hole. The pin is then secured in place using dental adhesive or cement. Once the pin is in place, the restoration can be attached to the pin using additional adhesive or cement.
Dentin pins are utilized in operative dentistry to retain a non-adhesive restorative material, thereby improving its stability within the cavity. Advantages of detin pins include:
- Enhanced retention: Dentin pins can significantly improve the retention of dental restorations, such as fillings and crowns, in situations where there is insufficient natural tooth structure to support the restoration. The pins provide an additional anchor point, helping to keep the restoration securely in place.
- Improved stability: By providing an anchor in the underlying dentin, dentin pins can help stabilize and distribute the forces applied to the tooth during biting and chewing, reducing the risk of restoration dislodgement or fracture.
- Conservation of tooth structure: In some cases, using dentin pins allows for a more conservative preparation of the tooth, preserving more of the natural tooth structure compared to alternative restoration methods.
- Adaptability: Dentin pins can be used with various types of restorative materials, such as amalgam, composite resin, and glass ionomer, making them a versatile option for dentists.
- Longevity: When used correctly, dentin pins can enhance the lifespan of dental restorations by providing a more secure and stable foundation, reducing the need for frequent repairs or replacements.
- Cost-effectiveness: In some instances, using dentin pins may be a more cost-effective option than other alternatives, such as dental posts or extensive crown preparations.
- Minimally invasive: Dentin pins are relatively small and minimally invasive compared to other types of anchoring systems, such as dental posts, which may require more extensive tooth preparation and removal of healthy tooth structure.
Despite the above advantages, dentin pin placement can also be a hazardous procedure, and several problems are associated with their use, including pulp damage, tooth fractures, inaccurate placement, infection, metal allergy, difficulty in removal, and limited use cases. In addition, dentin pins are not always necessary or appropriate for every situation. Therefore, alternative approaches, such as using a different type of restoration or building up the tooth structure with filling material, may provide better treatment options. Your dentist can help determine whether a dentin pin is necessary or appropriate for your specific dental needs.
Direct and Indirect Pulp Capping
Direct and indirect pulp capping are two techniques used in dentistry to treat teeth affected by decay or trauma but have not yet developed into a full-blown infection or abscess. The goal of both direct and indirect pulp capping techniques is to prevent the need for root canal treatment by preserving the vitality and health of the affected tooth. However, the success of the pulp capping procedure greatly depends upon the circumstances under which it is performed, and the prognosis depends on factors such as age, type, size, and the extent of pulp exposure.
The difference between Direct and indirect pulp capping is that:
- Direct pulp capping involves placing a dental material for capping directly on the site of pulp exposure. It is then covered with a protective layer, such as a filling or crown, to prevent further damage or infection.
- Indirect pulp capping involves removing the decayed or damaged tissue from the tooth, leaving a thin layer of affected dentin over the pulp. A biocompatible material is then placed over the affected dentin to stimulate the growth of new dentin and protect the pulp from further damage or infection. This material is also covered with a protective layer, such as a filling or crown.
Historically, the first pulp capping procedure was performed in 1756 by Phillip Pfaff. He used a small piece of gold to pack over an exposed vital pulp to promote healing. Nowadays, the material used for pulp capping is typically a biocompatible agent that can stimulate the growth of new dentin, the hard tissue that makes up the bulk of the tooth.
The ideal pulp capping material should have the following properties:
- Stimulate reparative dentin formation
- Maintain pulpal vitality
- Release fluoride to prevent secondary caries
- Be bactericidal or bacteriostatic
- Adhere to dentin
- Adhere to the restorative material
- Resist forces during restoration placement and throughout the life of the restoration
- Be sterile
- Be radiopaque
- Provide a bacterial seal
Various materials used for pulp capping include:
- Calcium hydroxide (Ca(OH)2): Introduced in 1921 by Hermann, it has been considered the “gold standard” of direct pulp capping materials for several decades.
- Zinc Oxide Eugenol (ZOE) Cement
- Corticosteroids and Antibiotics: Hydrocortisone, Cleocin, cortisone, Ledermix (calcium hydroxide plus prednisolone), penicillin, neomycin, and Keflin (cephalothin sodium) along with calcium hydroxide were used for pulp capping to reduce or prevent pulp inflammation.
- Collagen: Advocated as a pulp capping agent, as it is considered less irritating than Ca(OH)2, promotes mineralization but does not help in thick dentin bridge formation.
- Calcium phosphate cement: Suggested as a viable alternative due to its good biocompatibility, superior compressive strength, and its transformation into hydroxyapatite over time. It can help in bridge formation without superficial tissue necrosis and with a significant absence of pulp inflammation.
- Lasers:
- Carbon dioxide (CO2) (1W) laser used for direct pulp capping in 1985 by Melcer.
- Neodymium-doped yttrium-aluminum-garnet laser: Can be of therapeutic benefit for direct pulp capping and pulpotomy in clinical practice.
- Mineral Trioxide Aggregate (MTA): Studies have reported that MTA induces less pulpal inflammation and more predictable hard tissue barrier formation compared to hard-setting calcium hydroxide.
- MTA1-Ca: A resinous direct pulp capping agent containing calcium hydroxide, which can develop a dentin bridge without forming a necrotic layer and has good physical properties.
- BMP: Belonging to the Transforming Growth Factor beta (TGF-β) superfamily, BMP-2, 4, and 7 play a role in the differentiation of adult pulp cells into odontoblasts during pulpal healing.
- Recombinant Insulin-Like Growth Factor-I: Various growth factors, like epidermal growth factor, basic fibroblast growth factor, insulin-like growth factor II, platelet-derived growth factor-BB, and TGF-β 1, enhance reparative dentin formation in rat molars.
- Bone sialoprotein: A bioactive molecule that can induce homogeneous and well-mineralized reparative dentin. Both BSP and BMP-7 are superior to calcium hydroxide in their mineralization-inducing properties.
- Biodentin: A new bioactive cement with dentin-like mechanical properties, it has a positive effect on vital pulp cells and stimulates tertiary dentin formation.
- Enzymes like Heme-Oxygenase-1: They can play a cytoprotective role against pro-inflammatory cytokines and nitric oxide in human pulp cells.
- Statin: Known to induce angiogenesis and increase neuronal cells, it has an anti-inflammatory effect in various tissues and is considered an ideal active ingredient in pulp capping material to accelerate reparative dentin formation.
- Stem Cells: Dental Pulp Stem Cells (DPSCs) and Stem cells from Human Exfoliated Deciduous Teeth (SHED) have been identified as effective agents.
- Novel Endodontic Cement (NEC): Composed of calcium oxide, calcium phosphate, calcium carbonate, calcium silicate, calcium sulfate, and calcium chloride, NEC can form a thicker dentinal bridge with less pulp inflammation.
- Enamel Matrix Derivative (EMD): Secreted from Hertwig’s epithelial root sheath during porcine tooth development, EMD contains BMP-like molecules that promote odontoblast differentiation and reparative dentin formation. EMD-treated teeth have been reported to form more than twice the amount of hard tissue compared to calcium hydroxide-treated control teeth.
- Endo Sequence Root Repair Material: This material consists of calcium silicates, monobasic calcium phosphate, zirconium oxide, tantalum oxide, proprietary fillers, and thickening agents.
- Castor Oil Bean (COB) Cement: Comprising 81-96% triglyceride and considered a natural polyol containing three hydroxyl radicals, COB cement was originally developed as a biomaterial for bone repair and is an excellent candidate for pulp capping.
- TheraCal LC: A light-cured, resin-modified calcium silicate-filled liner designed for use in direct and indirect pulp capping, TheraCal LC serves as an insulator, barrier, and protectant of the dental pulpal complex under composites, amalgams, cement, and other base materials.
Both direct and indirect pulp capping are minimally invasive procedures that can help preserve the natural tooth structure and prevent the need for more extensive treatments, such as root canals or extractions. However, the success of these procedures depends on the extent and severity of the decay or trauma, as well as the overall health of the tooth and surrounding tissues.
Dentin Biomimetics and Tissue Engineering
Dentin biomimetics and tissue engineering are novel approaches for restoring and regenerating damaged dentin, the vital hard tissue covering the dental pulp. These advanced techniques aim to mimic the structure, function, and properties of natural dentin while utilizing cutting-edge technologies to create dental materials with superior qualities compared to existing ones.
Dentin biomimetics involves the development of new dental materials and approaches that closely resemble the native dentin in terms of its composition, structure, and biomechanical properties. These biomimetic materials aim to replicate the complex hierarchical organization of dentin, which consists of hydroxyapatite mineral crystals, collagen fibers, and water. The goal is to create restorative materials that interact seamlessly with the surrounding natural tissues, ultimately promoting better integration, biocompatibility, and long-term stability.
Tissue engineering is a multidisciplinary field that combines principles from biology, materials science, and engineering to develop functional substitutes for damaged or lost tissues. In dentistry, tissue engineering techniques focus on harnessing the regenerative potential of dental pulp stem cells (DPSCs) and other progenitor cells, as well as employing biomaterial scaffolds and signaling molecules to guide the formation of new dentin.
Key strategies in dentin tissue engineering include:
- Stem cell-based approaches: Utilizing dental pulp stem cells (DPSCs) or other progenitor cells to differentiate into odontoblast-like cells, which can produce new dentin tissue.
- Biomaterial scaffolds: Developing biocompatible and biodegradable scaffolds, such as chitosan/collagen matrices or hydrogels, that support cell attachment, proliferation, and differentiation while promoting mineralized matrix deposition.
- Signaling molecules and growth factors: Incorporating signaling molecules, such as bone morphogenetic proteins (BMPs) or transforming growth factor-beta (TGF-β), into the scaffold to stimulate and regulate the differentiation of stem cells into odontoblasts and promote dentin regeneration.
- Bioactive dental materials: Designing dental materials, such as mineral trioxide aggregate (MTA), calcium hydroxide, or Biodentin, that can promote tertiary dentin formation and improve the overall healing response in deep dental lesions.
By employing dentin biomimetics and tissue engineering techniques, researchers and dental practitioners strive to create innovative solutions for preserving and regenerating dentin, ultimately improving the long-term outcomes of dental restorations and minimizing the need for more invasive treatments such as root canals or extractions.
Dentin Regeneration and Growth Factors
Dentin is a vital hard tissue that covers the pulp and plays a crucial role in its protection. Any damage or loss of dentin may harm the pulp. Numerous studies and ongoing research aim to identify various agents that can aid in pulp regeneration.
Some critical growth factors and methodologies involved in dentin regeneration, include:
- Stem/progenitor cell-based tissue engineering can facilitate the regeneration of functional dentin. During dentinogenesis, new odontoblasts arise from perivascular cells identified by α-smooth muscle actin (αSMA) expression.
- A biomembrane, composed of a chitosan/collagen matrix embedded with calcium-aluminate microparticles can induce the differentiation of HDPCs into odontoblast-like cells, resulting in the deposition of a significant amount of mineralized matrix.
- Culturing DPSCs onto human-treated dentin (hTD) can regenerate dentin-like tissues. Similarly, fibrin has been proven to enhance pulp-like tissue generation and odontoblast differentiation, along with dentin sialoprotein expression.
- MTA or other experimental small molecules, such as GSK3 inhibitors, can promote tertiary dentin formation in deep dental lesions.
- Calcium hydroxide and Biodentin have also been reported to aid in the formation of tertiary dentin. Three capping materials, namely mineral trioxide aggregate (MTA), calcium hydroxide (CH), and Biodentin (BD), have been found to be biocompatible and stimulate the proliferation, migration, and differentiation of SHED.
- Nanofibrous spongy microspheres (NF-SMS) have been shown to provide dentin-like tissue formation with a remarkable level of mineralization.
- The application of bioprinting, combined with dental stem/progenitor cells using clinical methods of 3D fabrication, is currently suggested as an alternative to classical dental restorations for the regeneration of dental tissues. Bio-inks have enabled the synthesis of scaffolds with precise, reproducible microarchitectures. Novel dentin-derived extracellular matrix (ECM) hybrid cell-laden hydrogel bio-inks, synthesized from alginate and dentin matrix proteins, have been characterized and shown to have high printability and cell survival at different concentrations. Furthermore, these hybrid hydrogels demonstrated the ability to be embedded with acid-soluble dentin molecules, enhancing the odontogenic differentiation of SCAPs and effectively engineering the pulp-dentin complex.
- As previously mentioned, BMP-2 controls the odontoblastic differentiation of dental pulp stem cells, and transforming growth factor-β (TGF-β) can stimulate odontoblast-like cell differentiation and DPSC-mediated mineralization.
- Platelet-derived growth factor (PDGF-BB) and dentin-derived growth factors (eDMP) have been proven to enhance HDPSC proliferation and odontoblastic differentiation, generating dentin-like mineralized tissues.
- G-CSF has enhanced the proliferation and migration activity of stem/progenitor cells in dentin regeneration.
- The histone demethylation enzyme, lysine demethylase 1A (KDM1A), has been reported to regulate the directed differentiation in odontogenic MSCs by forming a KDM1A and PLOD2 (procollagen-lysine2, oxoglutarate5-dioxygenase2) protein complex. KDM1A in SCAP regulatory mechanisms of dynamic osteo/dentinogenic differentiation showed more diverse outcomes when applied in vitro than in vivo. However, KDM1A inhibition ultimately promoted osteo/dentinogenesis in vivo. Moreover, H2S has been proven to aid in the differentiation of DPSCs and dentin formation in vitro and in vivo via Ca2+ homeostasis and Ca2+ influx/GSK3β/(glycogen synthase kinase-3β) β-catenin cascade response. It is evident that β-catenin signaling plays a crucial role in dentin formation.
- Simvastatin (SIM), a drug commonly used to treat hyperlipidemia, has been reported to enhance odontogenic differentiation and accelerate mineralized tissue formation and de novo dentin formation.
- Small molecule inhibitors of glycogen synthase kinase 3 (GSK3), used in clinical trials for the treatment of neurological disorders such as Alzheimer’s disease, have stimulated reparative dentin formation, with naturally generated new dentin at sites of damage.
- Semaphorin 3A (Sema 3A) and its receptor Nrp1, typically expressed in rat dental pulp tissue and human DPSCs, are considered potent factors capable of inducing differentiation of DPSCs into odontoblasts. Sema3A application to dental pulp exposure sites in a rat model induced effective reparative dentin reconstruction and promoted the formation of an odontoblastic layer, dental tubules, and predentin.
In conclusion, dentin regeneration and growth factors play a vital role in preserving and restoring dental pulp health. Ongoing research in this field aims to develop more effective treatments and materials for dental restoration and regeneration, ultimately improving patient outcomes.
Dentin and Nutritional Factors
A variety of dietary factors are hypothesized to influence the health of teeth and their components. These factors include macro- and micronutrients, vitamins, pH properties, and behaviors associated with consumption. Additionally, factors such as the stage of development and specific medical conditions may define an individual’s nutritional status and its impact on oral health or vice versa. For example, older patients may experience tooth loss, reduced masticatory ability, and decreased appetite, which in turn, may influence their nutritional status.
To maintain optimal oral health, it is recommended to include the following vitamins and minerals in your diet:
- Calcium and vitamin D are two essential nutrients that play a critical role in maintaining the health of teeth and bones. Calcium is the primary mineral component of teeth and bones, while vitamin D helps the body absorb calcium from the diet. A deficiency in either nutrient can lead to weakened dentin and an increased risk of tooth decay.
- Phosphorus is another vital mineral for dental health, working together with calcium to strengthen teeth and bones. Good sources of phosphorus include meat, fish, poultry, dairy products, nuts, and legumes.
- Vitamin C is also essential for dental health, as it helps produce collagen, a protein that makes up the connective tissue in the body, including dentin in teeth. A deficiency in vitamin C can lead to weak and brittle teeth.
- Fluoride can help strengthen dentin by re-mineralizing the tooth structure, preventing tooth decay. Fluoride can be found in tap water (in regions with fluoridated water), toothpaste, mouth rinses, and some dietary sources like fish and tea.
On the other hand, certain food items should be consumed in limited quantities, such as sugar and acidic foods and drinks. These can negatively affect dentin health by promoting the growth of harmful bacteria in the mouth that can cause tooth decay.